JOHANNESBURG – Africa Health Exhibition & Congress 2018 is about to start. The event will take place in Johannesburg from 29th to 31st of May.
During the exhibition many topics on emergency medical filed will be discussed, and one of the speakers who will participate in this congress is Professor Andreas Engelbrecht, Consultant in Emergency Medicine at Steve Biko Hospital of Pretoria, as well as Adjunct Professor at the Division of Emergency Medicine at the University of Pretoria, South Africa.
We got in touch with him and we discussed about toxicology, cases of envenomation and relative medications. It is not so difficult to come up with a poisoning. Because of a snake bite, or maybe because of a plant or some mushroom. Causes can be several and various. Prof. Engelbrecht explained us how to treat such emergencies.
- What are the most common poisonings a person can come up with?
In our hospital patients present with poisoning from medications, street-drugs, alcohol and non-drug chemicals. The most common drug overdoses include paracetamol, sleeping tablets such as benzodiazepines and anti-depressants. Street drugs commonly abused are heroin, Nyaope which is a mixture of cheap heroin, cannabis and other chemicals such as anti-retrovirals that is smoked and stimulants such as metchathinone, commonly known as CAT and Metamphatmine which is commonly known as TIK. Non drug chemicals include pesticides such as organophosphates, corrosives and hydrocarbons such as paraffin also known as kerosene.
Because of the asymptomatic initial presentation of paracetamol overdose, a paracetamol level should be taken in most cases of drug overdose.
- Of course envenomations cannot be treated the same way. In case of snake bite, what are the medicines to administer? And, which are the symptoms for the patient in case of a venoumous bite?
There are around 160 snake species in Southern Africa of which about 16 are highly venomous.
Snake venoms are categorized as neurotoxic, cytotoxic and hemotoxic. Cytotoxic snakes such as the Puffadder (Bitis arietans) and Mozambican spitting cobra (Naja mossambica) are responsible for most venomous snake bites that require antivenom administration. Symptoms and signs include rapid and progressive swelling of the limb, blister formation, leakage of plasma and pseudo-compartment syndromes. Neurtoxic snakes such as the Black Mamba (Denroaspis polylepis) and Cape Cobra (Naja nivea) causes symptoms that are similar to the effects of the muscle relaxants used in anesthesiology. These symptoms include progressive respiratory muscle weakness, difficulty in swallowing, pupillary dilatation, slurred speech and droopy eyelids or ptosis. The full clinical syndrome is called progressive weakness.
Bites from hemotoxic snakes such as the Boomslang (Dispholidus typus) go asymptomatic for the first few hours. Thereafter patients develop a severe consumption coagulopathy with severe bleeding tendency. Patients bleed from the bite-wounds, under the skin to form large bruises, the gums, GIT, GUT and may also bleed into the brain.
Supportive care is very important for all snake bites.
- A Snouted cobra Naja annulifera brough along for identification after a bite
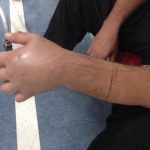
- Painful progressive swelling after a puffadder (Bitis arietans) bite
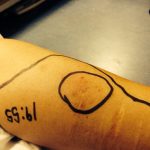
- Carefull assessment of the speed of swelling after an unknown snake bite
- Keeping trect of painful swelling after a snake bite
Careful attention must be given to the primary survey ABC. In Southern Africa, for the bite of 10 of the most venomous species, a polyvalent antivenom made of horse serum can be administered that can be life and tissue saving. Preparations for airway management and anaphylaxis must be made before initiating antivenom therapy. A dose of six to eighteen vials will be administered diluted into normal saline and given over 30 minutes depending on the type and severity of the envenomation. Higher doses are necessary for bites of highly neurotoxic snakes like the Black mamba and the Cape Cobra. There is no pediatric dose as children are envenomated by the same amount of venom as adults. Because the horse serum is highly allergenic, 0.25mg of adrenaline should be given S/C prior to antivenom administration. This intervention has been proven to be effective in reducing allergic reactions by as much as 40%. It is important in atopic individuals but must be weighed carefully in patients with uncontrolled hypertension, ischemic heart disease or with a tendency to arrhythmias. Antihistamines and corticosteroids are not effective prophylaxis. A booster of anti-tetanus toxoid vaccination should always be given to victims of snake bite. For the hemotoxic Boomslang monovalent antivenom is available.
- Regarding, mushroom poisoning: are there different types of mushrooms that cause poisoning? Which are the symptoms and how do you act in such cases?
There are more than 10 000 species of mushrooms of which 50 to 100 are potentially poisonous. Most deaths from mushroom poisoning are caused by one species of mushroom called Amanita phalloides. These large light brown to greenish mushroom grows in forests near oak and pine trees. The have a deceptively delicious taste. Patients are initially asymptomatic for up to 24 hours. This delay in symptom onset is very characteristic of this type of mushroom poisoning compared to other poisonous mushrooms in which symptoms will start as early – within 30minutes to two hours. Patients then develop a profuse food poisoning type diarrhea. If the history of mushroom poisoning is not identified patients are often discharged after rehydration. A honeymoon period of 24 to 48 hours follows and thereafter patients return with fulminant hepatic failure.
Careful attention should be given to supportive care. Intravenous lines should be inserted and the patient should be well hydrated to ensure adequate urine output.
Patients who present early should be given multiple doses of activated charcoal. Activated charcoal powder can be given in a dose of 1g per kg mixed in water. If the patient finds it hard to swallow, it can be made more palatable by mixing it in coca cola or chocolate mousse. It can also be administered via naso-gastric tube but patients should be intubated to avoid aspiration if they have a decreased level of consciousness.
The risk of aspiration should always be weighed against the benefit of potential decreased absorption of the poison.
Follow up doses of 0.25g per kg can be given every 1 to 2 hours for the next 4 to 6 hours. Check bowel sounds before each dose. Activated charcoal should not be given to patients with ileus or active vomiting.
The antidote for amatoxin, the poisonous substance in Amanita phalloides is Silibinin which should be administered IV in a loading dose of 5 mg /kg. It should be followed with a dose of 20 mg /kg via continuous infusion over 24 hours.
Other antidotes that may be considered include high doses of penicillin and N-acetyl-cysteine (NAC).
Amanita phalloides is not the only poisonous mushroom. Other poisonous mushrooms include are Amanita muscaria – red cap with white spots. It contains muscimol that leads to anticholinergic symptoms. Management is supportive. Psilosybin mushrooms, better known as “magic mushrooms” or “shrooms” contain psychoactive psilosybin with effects similar to LSD. It appears to work on the serotonergic system and cause feelings of euphoria but can also cause hallucinations and hyperthermia. If patients are intoxicated they should be managed supportively and given a benzodiazepine to calm them down if necessary. Coprinus mushrooms have an inky cap. They can be poisonous if taken with alcohol and cause a Disulfiram type reaction. Management is supportive.
- Poisoning can be caused also by plants. In case of anticholenergic poisoning from plants, what are the symptoms and the correct treatments?
Plant poisonings are very common. Most of these poisonings are mild and accidental. Usually when children explore the world with their mouths and sample pieces of plant material. More severe poisonings can occur when adults deliberately ingest larger quantities of plants as wild food or for the perceived mind altering effects.
Anticholinergic poisoning is common in the latter group of cases. Examples of plants with anticholinergic effects are Atropa belladonna and Datura stramonium. Patients will present with the anticholinergic syndrome which can best be remembered by the following mnemonic:
- “Blind as a bat” – pupillary dilatation
- “Mad as a hatter” – central acting anticholinergic effects
- “Hot as a hare” – inhibition of sweat production and vasodilatation
- “Red as a beet” – vasodilatation
- “Dry as a bone” – axillae are dry and it’s an important way to distinguish this toxidrome from stimulants
- “Full as a flask” – urinary retention
- “Fast as a pink flamingo” – tachycardia
When patients present with this toxidrome they should be calmed down and talked down. An IV line should be inserted and a benzodiazepine given to further calm the patient down. If the patient presents within two hours activated charcoal can be considered for decontamination.
The antidote for this poisoning is Physostigmine. 0.5 to 1mg can be given IV over 5 minutes. It is very effective for anticholinergic syndrome with central nervous system effects. It should NEVER be given if the anticholinergic syndrome is caused by drugs with that cause multiple receptor blockades such as tricyclic antidepressants. In such cases Physostigmine can cause severe bradycardia or precipitate seizures. Always do an EKG and evaluate the width of the QRS complex which should be < 100ms.
- Brugmansia arborea contains atropine and scopolamine and causes anticholenergic syndrome when it is used to infuse home brewed teas
- Nerium oleander is a poisonous plant that contains cardiac glycosides
- Datura stramonium – all parts of the plant is poisonous and contains atropine and scopolamine
- In order to avoid envenomations, which precautions people should bear in mind before having walks and day trips in the nature?
City dwellers are a little out of sorts in nature. Here are a few tips:
Develop awareness. Awareness is the ability to notice things in your surroundings. Consider the direction that you are walking in and look for landmarks such as trees or hills that will help you if you get lost. Take notice of the plants and animals that surrounds you.
If you visit a country with venomous snakes or scorpions, it is important to wear closed shoes to protect your ankles from sprains but will also offer some protection from bites and stings. You may even choose to wear leggings.
Do not approach or touch wild animals even if they look tame. Keep a safe distance. Report to a medical facility if you got bitten by a snake, insect, tick or animal or if you are stung by a scorpion.
Do not eat any plant material if you do not know exactly what it is. If you are lost and in a life or death survival situation, you should taste a small part of a berry before eating it. If the color is red and it tastes very sweet it’s usually ok to eat. If it’s bitter or have an unpleasant taste, stay away from it. Do not eat mushrooms unless you bought them from the supermarket.
- You will be a speaker during Africa Health Exhibition & Congress 2018. What will be the your intervention during the show?
I will be presenting an update on the management of snake-bite. I will also talk about scorpion sting and spider bite. Lastly I will be participating in a panel discussion on poisoning and toxicology in general.